Walsh, Colin G.; Ripperger, Michael A.; Novak, Laurie; Reale, Carrie; Anders, Shilo; Spann, Ashley; Kolli, Jhansi; Robinson, Katelyn; Chen, Qingxia; Isaacs, David; Acosta, Lealani Mae Y.; Phibbs, Fenna; Fielstein, Elliot; Wilimitis, Drew; Musacchio Schafer, Katherine; Hilton, Rachel; Albert, Dan; Shelton, Jill; Stroh, Jessica; Stead, William W.; Johnson, Kevin B. “Risk Model-Guided Clinical Decision Support for Suicide Screening: A Randomized Clinical Trial.” JAMA network open, vol. 8, no. 1, 2025, e2452371, https://doi.org/10.1001/jamanetworkopen.2024.52371.
Suicide prevention involves identifying individuals at risk, intervening when necessary, and providing follow-up care. Traditionally, identifying suicide risk has relied on patients sharing their own concerns, reports from their support network, or in-person screenings. While statistical models have been developed to help identify those at risk, these models are not always used in real-world clinical settings. Some challenges to implementing these models include the stigma surrounding suicide and uncertainty about how best to integrate them into routine healthcare practices.
This study aimed to test the effectiveness of a system that uses a statistical risk model to prompt healthcare providers to assess suicide risk. The trial, conducted from August 2022 to February 2023, involved patients at Vanderbilt University Medical Center. The study compared two types of decision support systems: one that interrupted the healthcare provider with an alert and another that simply displayed an icon with information about the patient’s suicide risk. Both systems used a real-time, validated model to assess suicide risk.
The results showed that the interruptive system, which triggered an on-screen alert, led to more healthcare providers deciding to conduct a suicide risk assessment compared to the noninterruptive system, which only displayed an icon. Specifically, 42% of encounters with the interruptive system resulted in a decision to screen for suicide risk, compared to only 4% with the noninterruptive system. There were no reported cases of suicidal thoughts or attempts during the study.
In conclusion, the study found that an interruptive decision support system was more effective in prompting healthcare providers to assess suicide risk than a noninterruptive one. This suggests that using such systems in healthcare settings could help prevent suicide, and further research is needed to test whether these systems can effectively reduce self-harm.
Figure 2. Participant Flow Diagram
BPA indicates best practice alert; CDS, clinical decision support; and CSSRS, Columbia Suicide Severity Rating Scale.
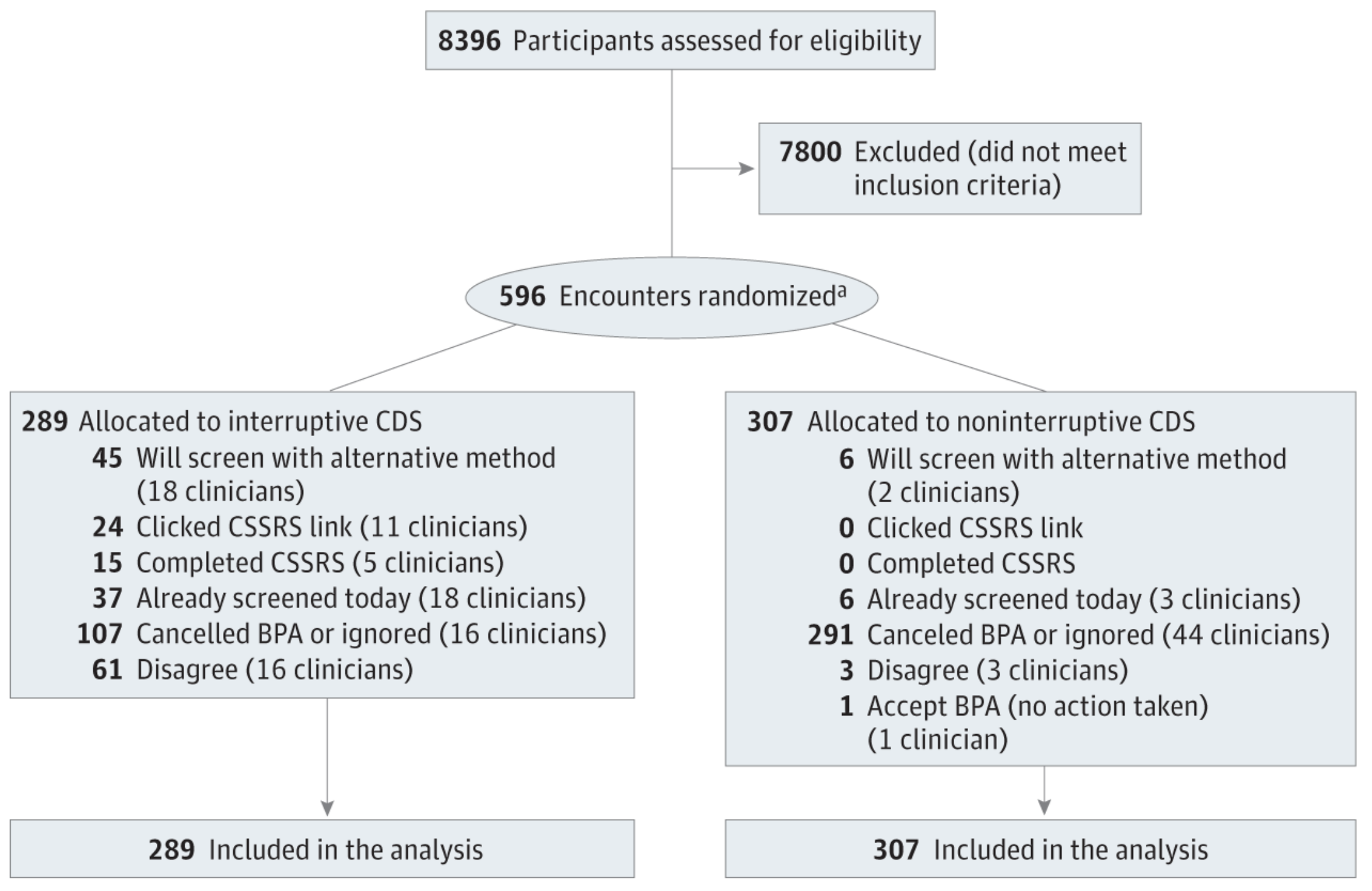
aIncludes 561 patients with first encounters and 72 clinicians.